Twenty-three Michigan residents were accused of illegal fraudulent schemes that involved defrauding Medicare of more than $61.5 million by billing Medicare for unnecessary medical services that were never administered and by paying kickbacks and bribes, according to official reports.
“As alleged, the defendants and their co-conspirators repeatedly paid illegal bribes and kickbacks so they could submit claims for medically unnecessary home health services throughout the Detroit metropolitan area, exposing patients to needless physician services and drug testing and costing Medicare tens of millions of dollars,” said Assistant Attorney General Kenneth A. Polite, Jr. of the Justice Department’s Criminal Division. “As these actions demonstrate, we will work tirelessly to tackle complex, illegal schemes that take advantage of vulnerable populations and defraud federal programs of taxpayer dollars meant to provide health care to millions of Americans.”
Two Oakland county residents, Walid Jamil, 62, and Jalal Jamil, 69, owned and operated numerous home health agencies around Metro Detroit, according to court documents. Allegedly, they concealed their ownership of these agencies by using their family members and others as straw owners. They submitted around $50 million in fraudulent home health care claims to Medicare. They also allegedly paid bribes for patient recruiting, but these patients were not in need of home health care, did not meet the qualifications for home health care and oftentimes did not receive the care Medicare was billed for, according to reports.
Walid and Jalal Jamil allegedly assembled quid pro quo relationships with physician clinics to obtain the necessary information to fraudulently bill Medicare, according to official reports by the Department of Justice. This lead them to receive more than $43 million from Medicare and these funds were misappropriated.
“The alleged actions of these defendants is an astonishing abuse of our health care system,” said U.S. Attorney for the Eastern District of Michigan Dawn N. Ison. “By allegedly submitting fraudulent claims and paying illegal kickbacks, these defendants looted Medicare in order to line their own pockets at great cost to taxpayers. My office is grateful for the continued work of the Health Care Fraud Strike Force to root out corrupt medical professionals.”
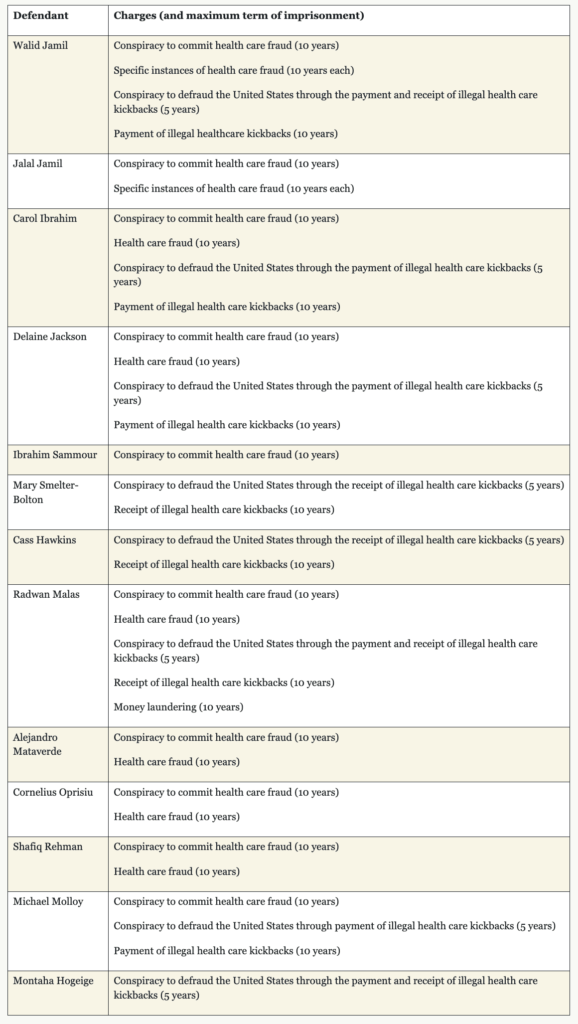
Source: U.S. Department of Justice
Employed by the Jamil home health agencies, Carol Ibrahim, 45, an Oakland County resident, and Delaine Jackson, 48, a Wayne County resident, allegedly illegally paid patient recruiters and submitted fraudulent claims to Medicare. According to reports, Ibrahim is also an alleged straw owner of one of the Jamil home health agencies.
The agencies also employed Ibrahim Sammour, 62, a registered nurse and Wayne County resident. Sammour allegedly billed Medicare fraudulently for home health services that he never provided as well as wrongly certified patients as “homebound.”
Alleged recruiters, including Mary Smelter-Bolton, 69, of Oakland County and Cass Hawkins, 52, of Wayne County, were allegedly paid by various Jamil home health agencies to refer patients on Medicare for home health services. These services were billed to Medicare even though the claims did not have the eligibility of reimbursement, according to Department of Justice reports.
According to court documents, Radwan Malas, 43, of Oakland County started operating Infinity Visiting Physician Services PLC, a home visiting physician company, in 2015. Through this company, he allegedly would enforce that the doctors he employed had to certify patients referred by Walid Jamil and Jalal Jamil for medically unnecessary home health services. He allegedly billed Medicare for various services that these patients never received, including 60-minute complex patient visits and injections of B-12 and toradol. Malas also allegedly forced his employed physicians to order the highest-reimbursing urine drug test. He then allegedly received a referral fee from the labs that processed the samples.
According to reports, the defendants billed Medicare for more than $11.5 million in fraudulent claims for which they received roughly $4 million, which was misappropriated. It is also alleged that Malas laundered the funds by organizing illegal financial transactions.
“At the FBI, we swear an oath to protect the American people,” said Assistant Director Luis Quesada of the FBI’s Criminal Investigative Division. “Fraudsters look to orchestrate their schemes at the cost of our health care systems, patients and taxpayers. The FBI and our law enforcement partners remains dedicated to investigating and bringing to justice those who seek to exploit our U.S. healthcare system at the expense of its patients.”
Several medical professionals, including Dr. Alejandro Mataverde, 79, of Oakland County, Dr. Cornelius Oprisiu, 82, of Livingston County and nurse practitioner Shafiq Rehman, 59, of Wayne County, were employed by Infinity. They allegedly administered medically unnecessary services to Medicare beneficiaries or submitted claims to Medicare for medical services that were not administered to the patients.
“Those who attempt to defraud Medicare often do so at the risk of compromising the integrity of federal health care programs and disregarding the health and wellbeing of patients,” said Special Agent in Charge Mario Pinto of the Department of Health and Human Services Office of Inspector General (HHS-OIG). “HHS-OIG is proud to work alongside our law enforcement partners to protect federal health care programs and hold bad actors accountable for their actions.”
Michael Molloy, 50, of Wayne County, was co-owner of Integra Lab Management LLC, which processed the high-reimbursing and allegedly medically unnecessary urine tests submitted by Infinity. Molloy and his co-owners allegedly paid the salary of Infinity employees and made monthly payments to Malas in exchange for the doctor orders for the urine drug testing that was medically unnecessary. The illegal kickbacks resulted in approximately $2.8 million in fraudulent claims to Medicare submitted by Integra and they were paid more than $730,000 according to official reports.
A medical assistant employed by Infinity, Montana Hogeige, 39, of Wayne County, allegedly agreed to accept her salary from Integra as an illegal kickback to Infinity in exchange for doctor orders for the high-reimbursing urine drug tests.
“Medicare is designed to provide vital government funded services to our people. It is not a slush fund for thieves and fraudsters,” said Acting Special Agent in Charge Charles Miller of the IRS Criminal Investigation (IRS-CI) Detroit Field Office. “IRS-CI will work tirelessly with our law enforcement partners to investigate those who illegally target our Medicare program for personal financial gain.”






Leave a Reply